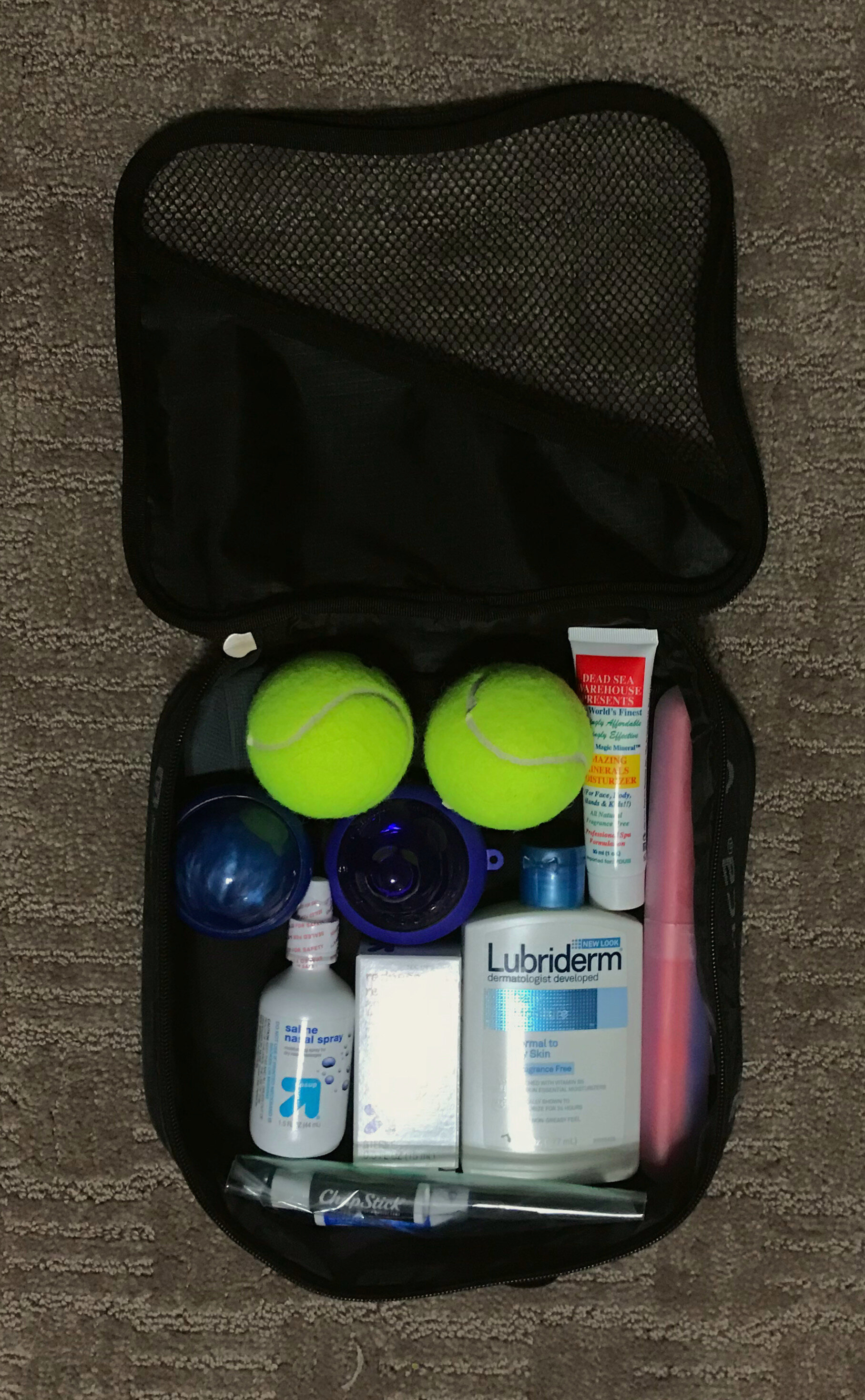
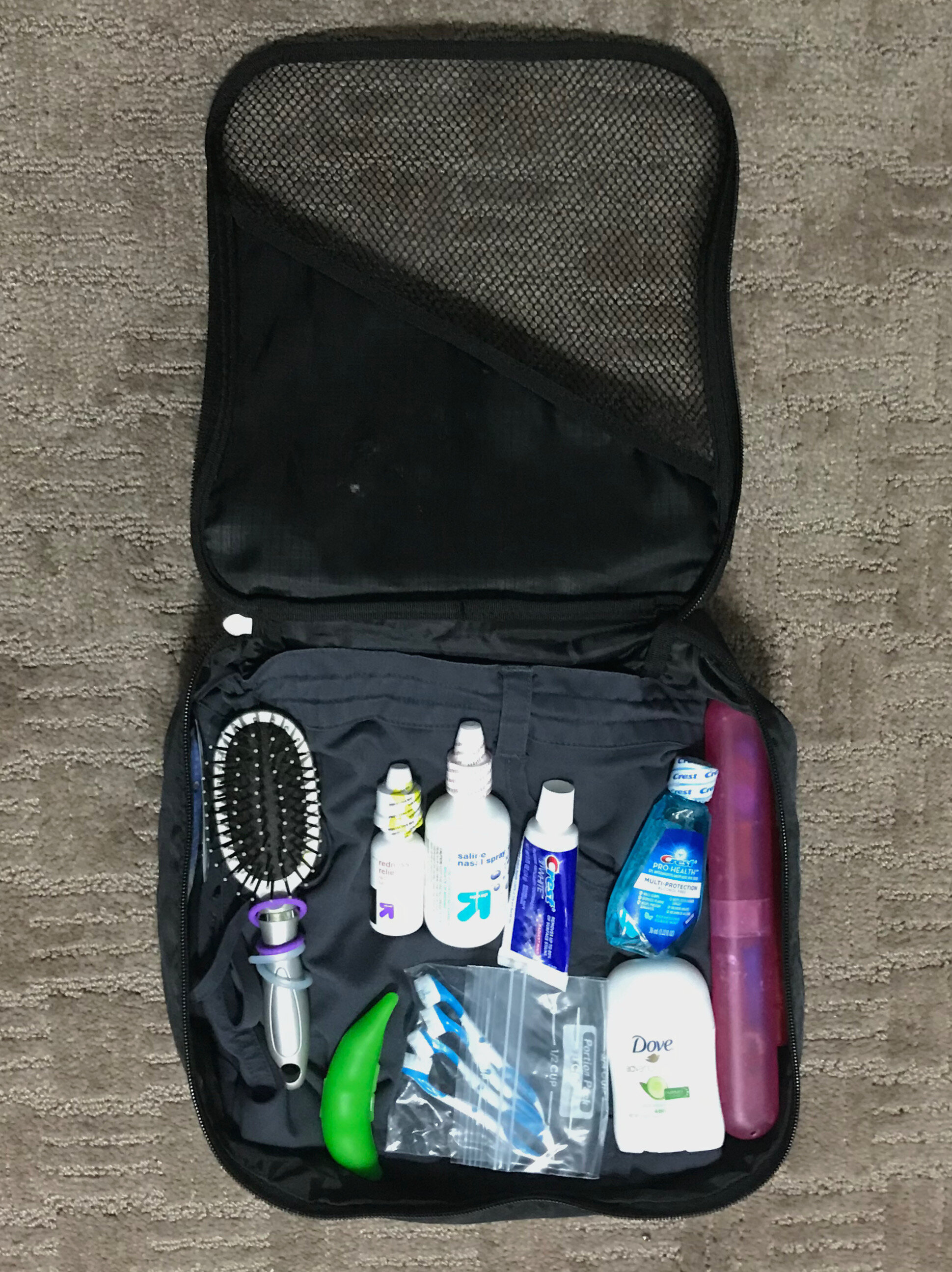
After receiving the call that she had given birth, we made plans for me to come to their home and start the process that evening. As usual, I arrived and began cleaning, sanitizing, and setting up. My client and her mother wanted to watch the whole process, so they set up camp at the breakfast bar above my work area. As I began working, my client began taking photos, and let me know she was posting them on her SnapChat. I thought it was a fun idea, and figured it might reach 20 or 30 people.
Little did I know, the snaps were also posted to Facebook, and quickly began being shared. The first time I knew this was going to be a crazy ride was when I saw the post had 8,000 shares. I shared this with fellow placenta professionals, and we celebrated and wondered what this would turn in to. Little did I know, in just a few days, the original post would reach 100,000 shares. I began receiving private messages and comments that weren't so great, and had to lock down my personal page and carefully monitor my business page. I have received some great encouragement and support, but have also learned that people can be incredibly hateful when hidden by a screen.
The content was soon picked up by an agency and was posted on the Daily Mail, the Sun, Metro, and the Mirror! I'm not sure exactly how far this little video reached, as it has been re-posted in other formats, on pages, in groups, on websites, and who knows where else! I could not have imagined this happening, in my mind it was just little ol' me doing my job! I look forward to helping mothers consume their placentas however they desire for years to come.